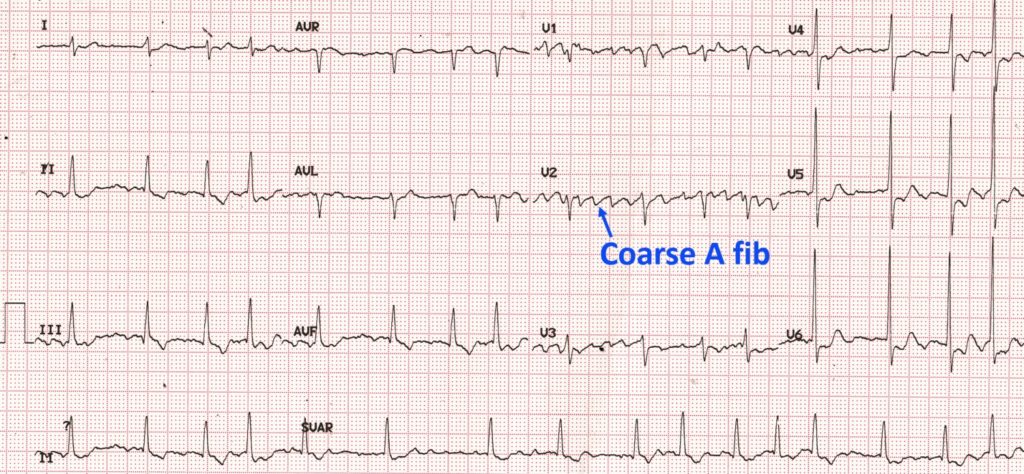
It appears there are different triggers so just have to be aware of each episode and what might have triggered it. In the ER I’ve always had low potassium phosphate and chloride. I also get a pain on the left side of my upper abdomen left of xiphoide. I’m looking for answers for underlying reason for Afib especially with RVR. My cardiologist says I’m the healthiest patient he has ever had but that doesn’t take away the worry and concern. That’s my norm however I feel bradycardia is indictative of Afib. Only complication is exposure to 9/11 and must where Cpap despite ideal weight and BMI. Don’t do caffeine or alcohol and avoid medications that are stimulants or depressants. First several short episodes happened in my 20s but never during exercise. Engage in strength training yoga, and now walking only (no running) Afib occurs about 1-2 times a year since 2011 always in January or February where it is prolonged enough to visit ER with spontaneous conversion or with meds. Active 48 years with perfect blood pressure, perfect cholesterol and no diabetes. This is still an area for research and further information will be needed before this can be used routinely in the clinic. One recent development is the awareness of increased activity of the If channels which raises the possibility that blockade of these channels with ivabradine might have an anti-arrhythmic in vagal AF patients. In contrast there are no specific studies reporting the success of ablation in vagal AF. The pulmonary veins are a well-recognised source of AF in many patients and ablation can be effective in reducing paroxysmal AF. These drugs include flecainide, quinidine, and disopyramide. Alternative drugs such as those which reduce vagal tone should theoretically be effective. Drugs which block the sympathetic nervous system commonly used in the management of AF such as beta blockers and digoxin should be avoided. With respect to reducing vagal AF episodes there are only anecdotal data about the best way to manage this. How should vagal AF be managed? Anticoagulation as per the underlying stroke risk predicted by CHAD2VASC score should be considered. Vagal stimulation shortens atrial effective refractory period and augments the ability of a single atrial premature beats to induce AF. One way is to assess heart rate variability which can assess the balance between the sympathetic and parasympathetic or vagal tone. It is possible to measure the activity of the autonomic nervous system but it is difficult. The ventricular rate during the AF is generally not fast. ECG recordings often show a combination of atrial flutter alternating with atrial fibrillation. When a 24h ECG monitor is performed sinus bradycardia usually occurs before the onset of the AF. If the patient participates in endurance sports such as cycling, marathon running or cross country skiing then AF is also more common. Vagal AF is more frequently seen in younger patients (30-50 years old), typically men and usually the heart is structurally normal on echocardiography. Commonly this type of AF stops in the morning or during periods of exercise and can be precipitated by cough, nausea, after eating, swallowing and ingestion of cold foods and drinks. When to suspect vagal AF: If the arrhythmia occurs at rest, after meals or during sleep then it is more likely to be vagal stimulated. So called vagal AF is enigmatic but should be more recognised. This is important because it needs to be managed differently from other more common types of atrial fibrillation. For some patients increased vagal activity is associated with the initiation of atrial fibrillation. It is part of the autonomic nervous system and its cardiac action is to slow the heart. The vagus nerve wanders from the brainstem throughout the chest and abdomen innervating the heart, lungs and intestines. The initiator of the AF episodes can often be overlooked in the consultation but is very important particularly as vagal AF will gets worse when treated with beta blockers. 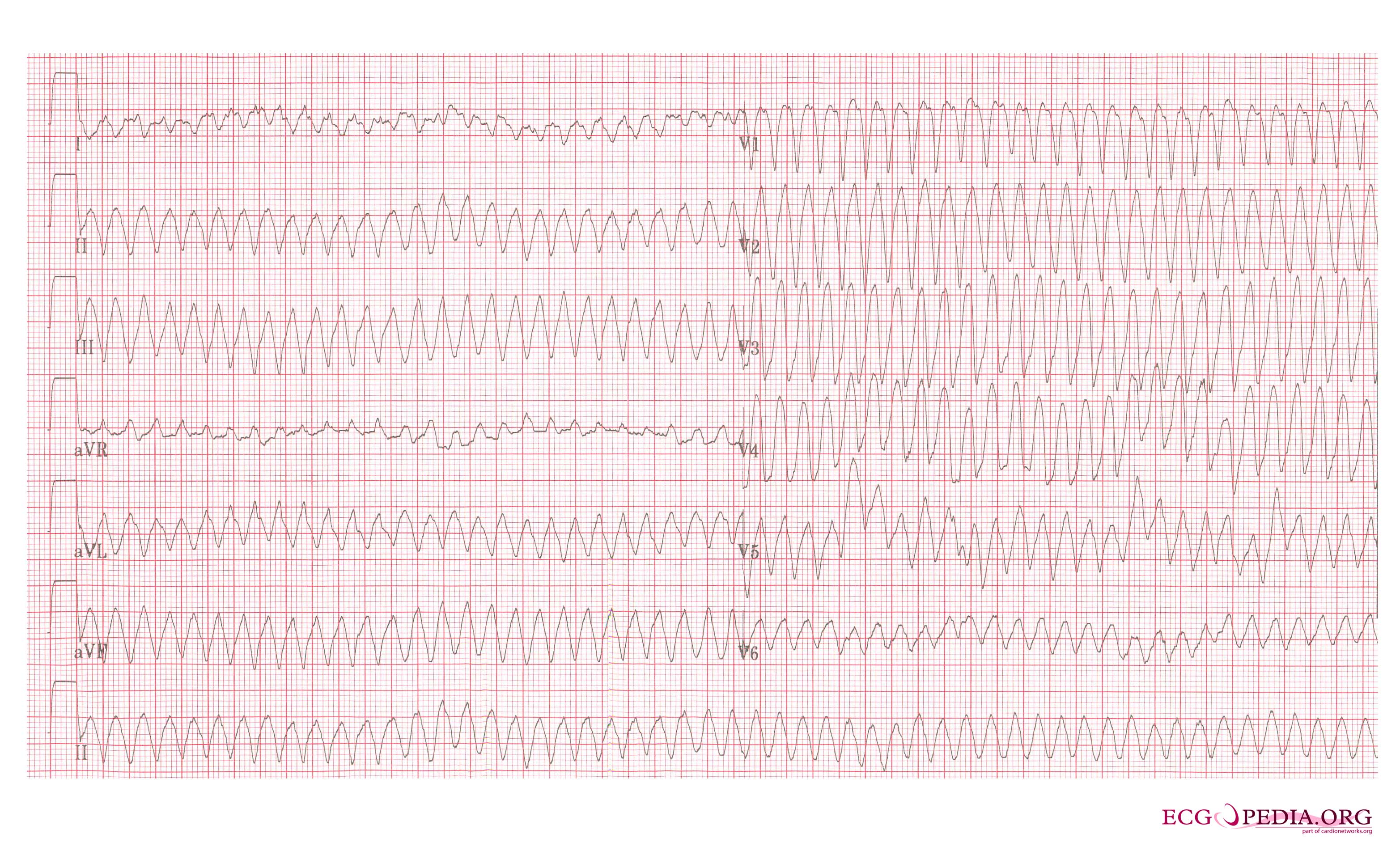
Another way of classifying AF is Sympathetic or adrenergic AF and vagal AF. These things are definitely associated with AF but what triggers episodes. When they are asked about the causes of AF they will usually list high blood pressure, ischaemic and valvular heart disease, alcohol and over active thyroid. When doctors are asked to classify atrial fibrillation (AF) they usually start by describing it as paroxysmal (coming and going) or persistent.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
